A 68-year-old African American male presented with a nontender mass under his tongue for 2 weeks. He had dysarthria because of compromised tongue movement. He denied pain, bleeding, dysphagia, loss of appetite, weight changes, and shortness of breath. There was no history of prior swelling, trauma, or oral cavity surgeries. Clinical examination revealed a mobile, solid, non-tender, oval-shaped right sublingual mass (3.0 x 2.0 cm). No notable cervical adenopathy was found.
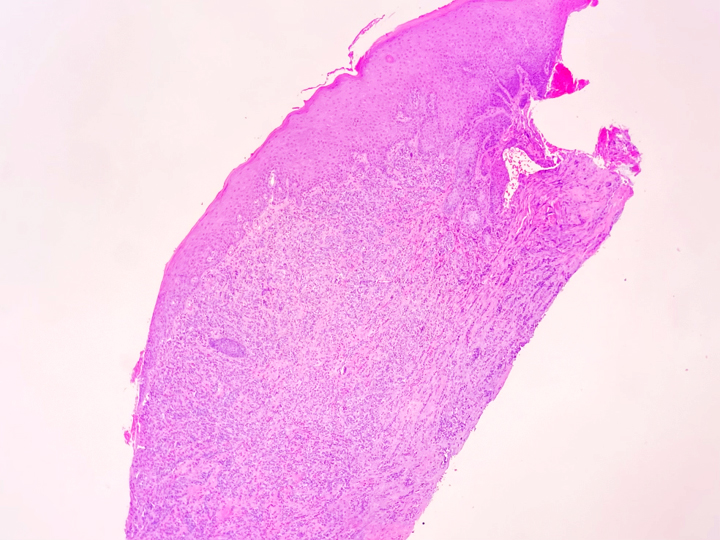
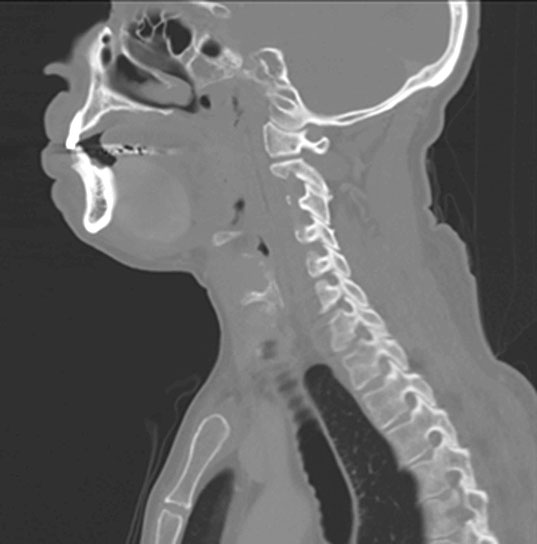
CT scan showed a well-circumscribed, oblong shaped hyperdense mass (4.1 x 2.5 x 4.0 cm) situated within the floor of mouth/right sublingual gland with mild mass effect upon the midline intrinsic tongue musculature. No calcification or sialolith were identified. There was no surrounding inflammation or cervical lymphadenopathy. Excision of the mass was performed.
Q1. Which genetic alteration is associated with this tumor?
Q2. Histologic features of the tumor always predict outcome in these patients.
Solitary Fibrous Tumor (SFT)
Solitary fibrous tumor (SFT) is a rare soft tissue tumor of mesenchymal phenotype. Originally described in the pleura by Klemperer and Rabin in 1931, these tumors have represented a unique diagnostic and treatment challenge. SFT may be found in almost any site of the body with the intrathoracic location being the most common. Other locations include the trunk, extremities, head and neck, and intracranial. Those in the head and neck may arise in the sinonasal tract, oral cavity, larynx, or orbit. In the oral cavity, buccal mucosa is the most common location. Less than 10 cases have been reported in the floor of mouth.
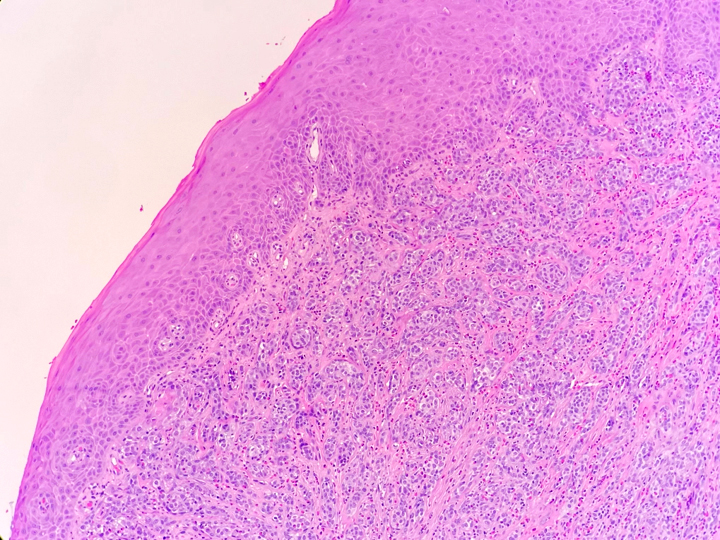
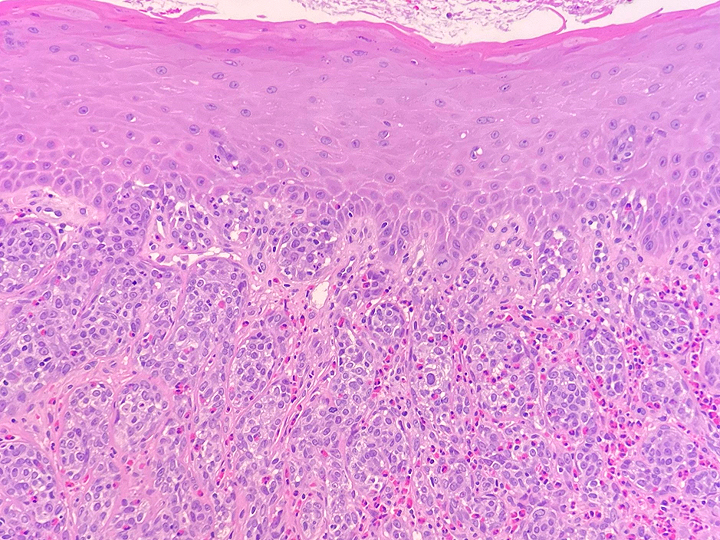
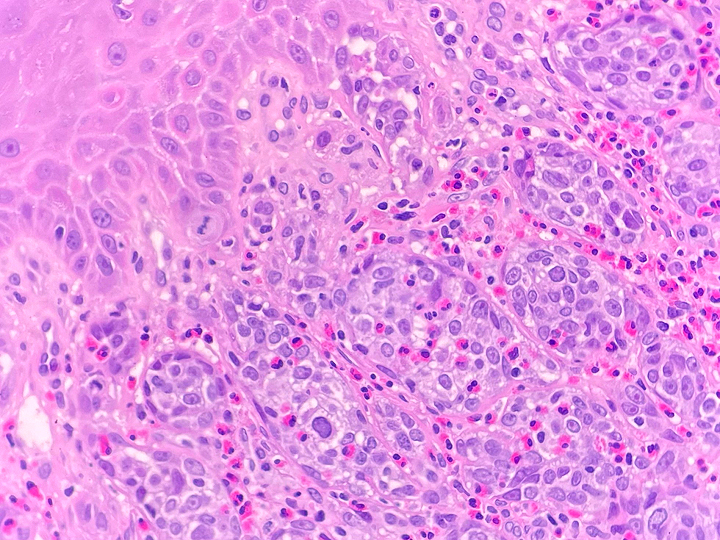
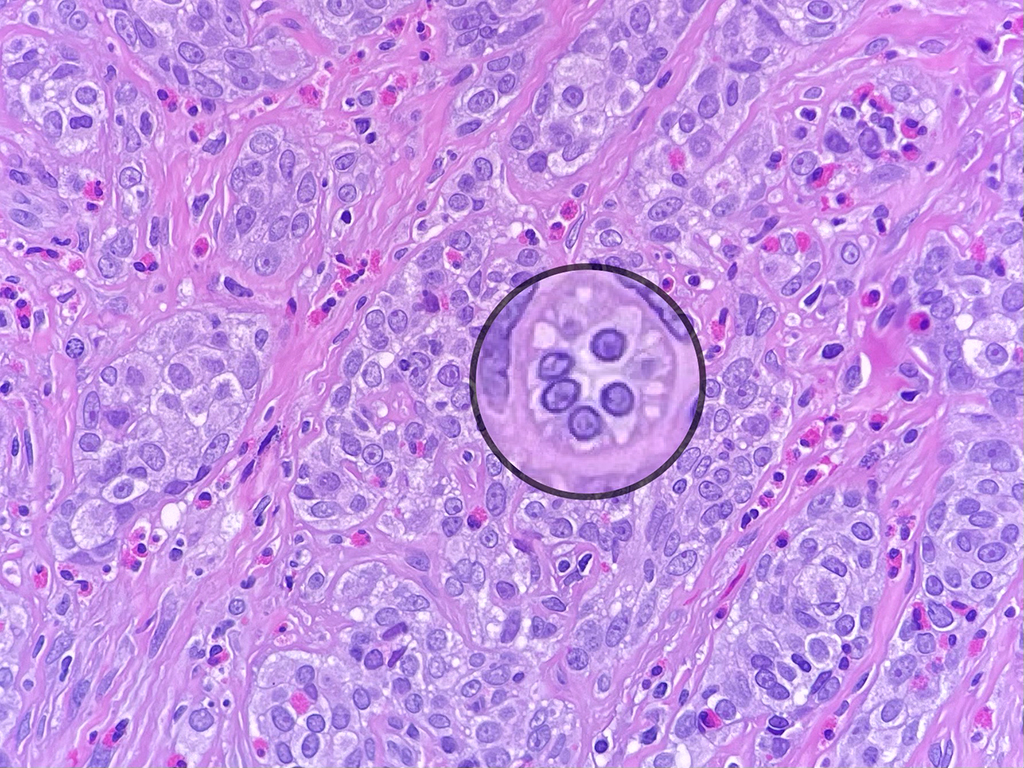
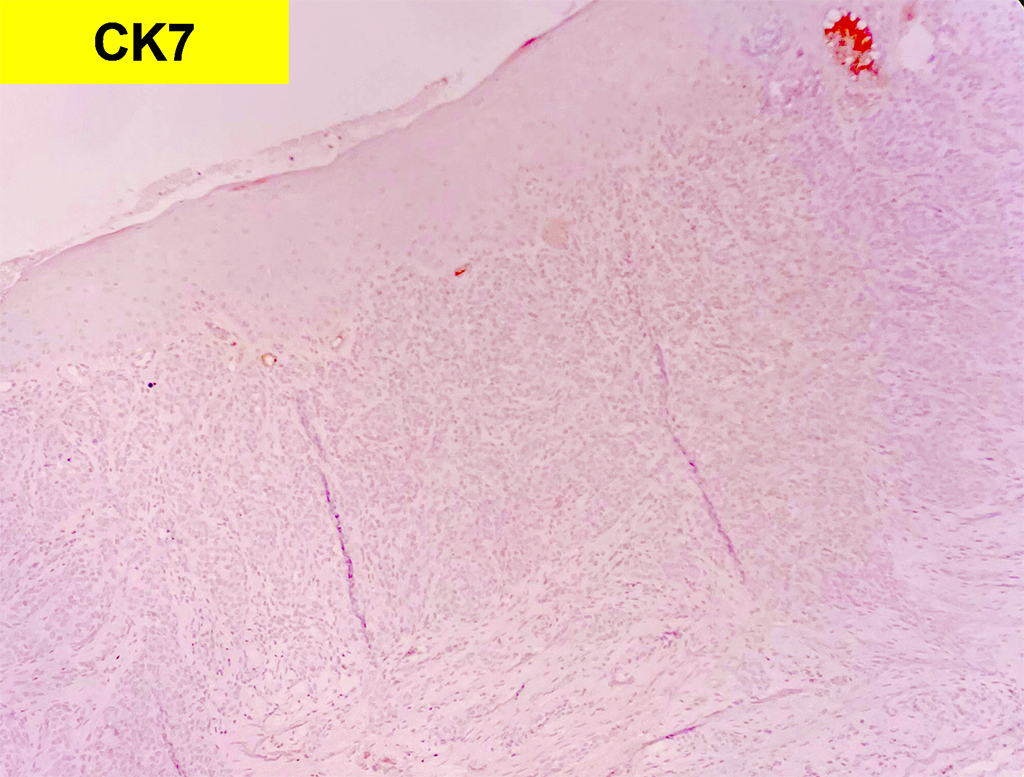
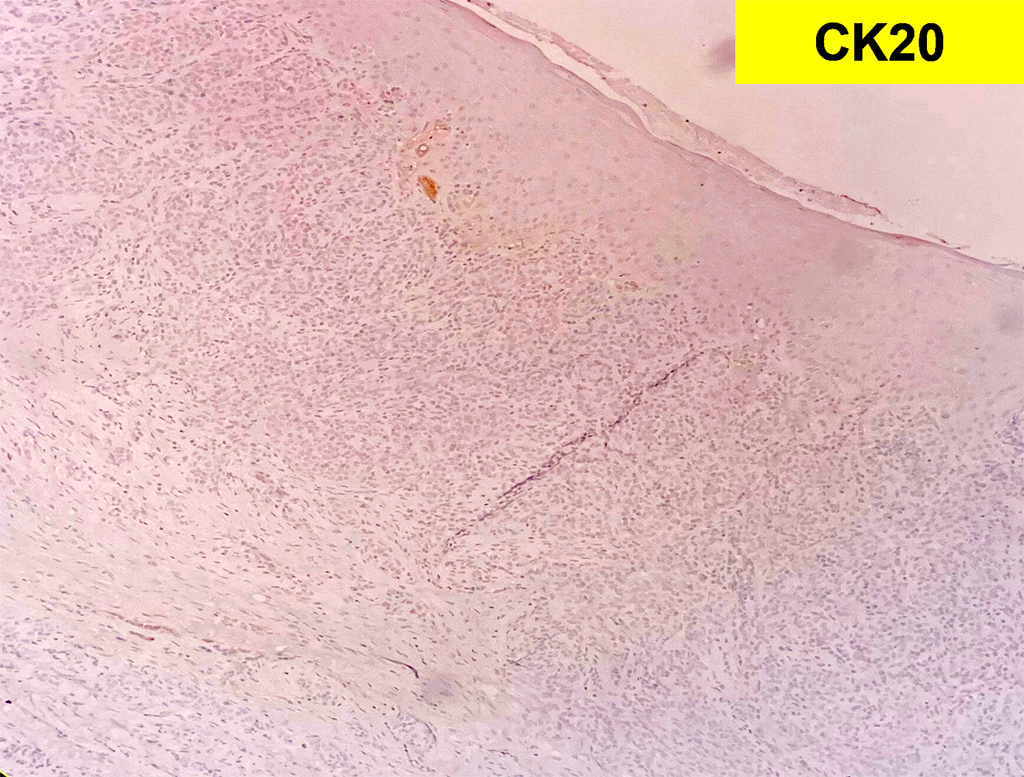
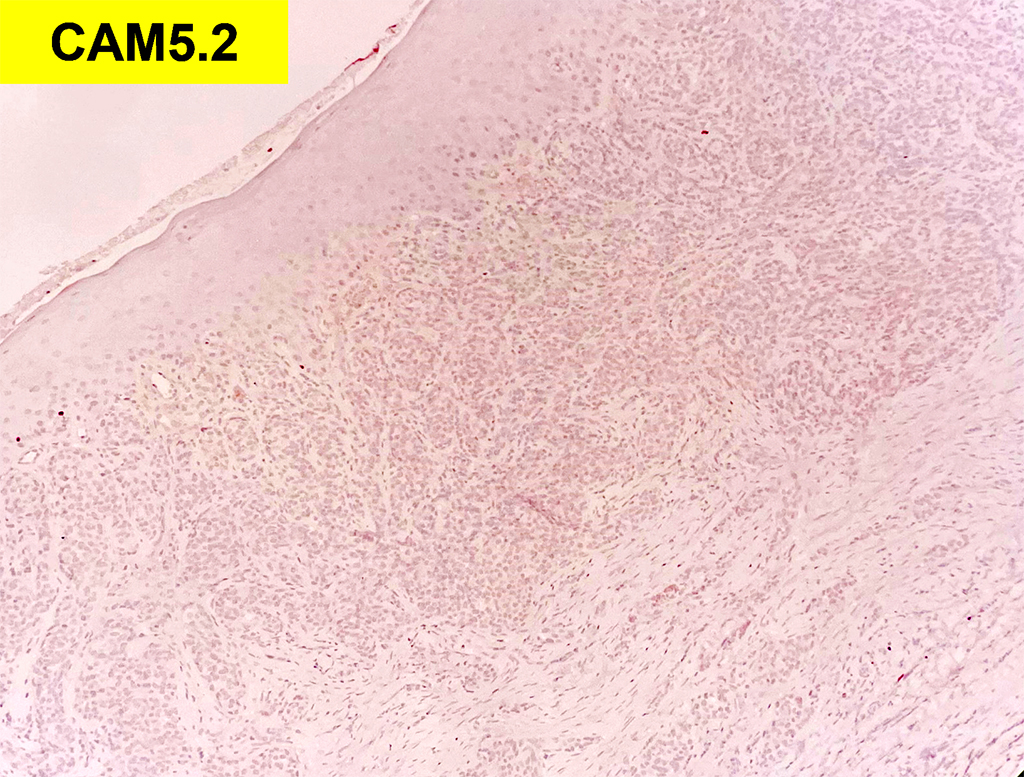
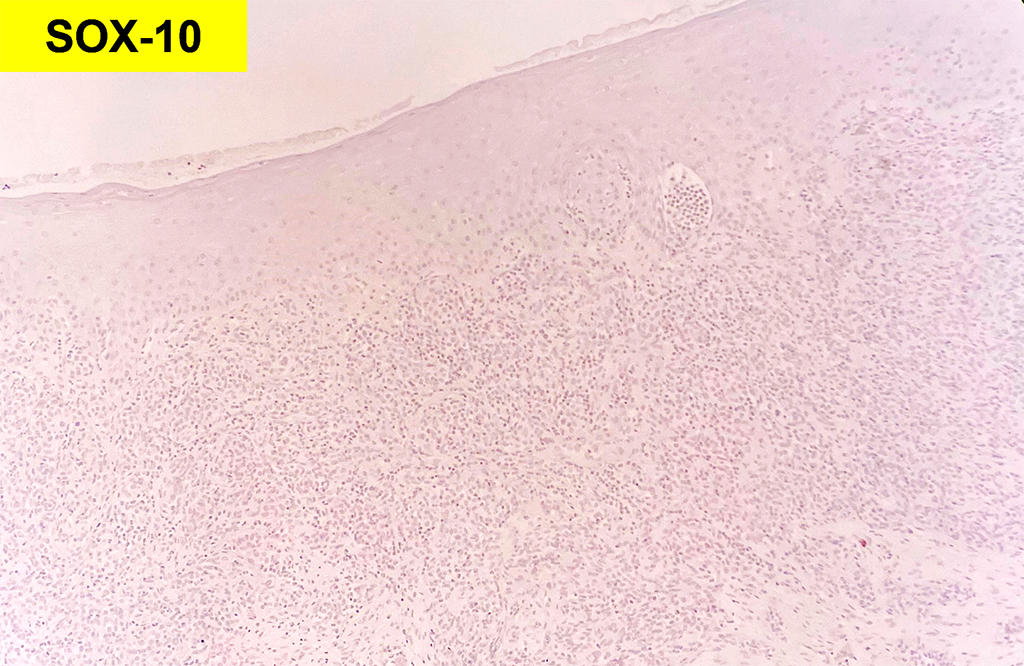
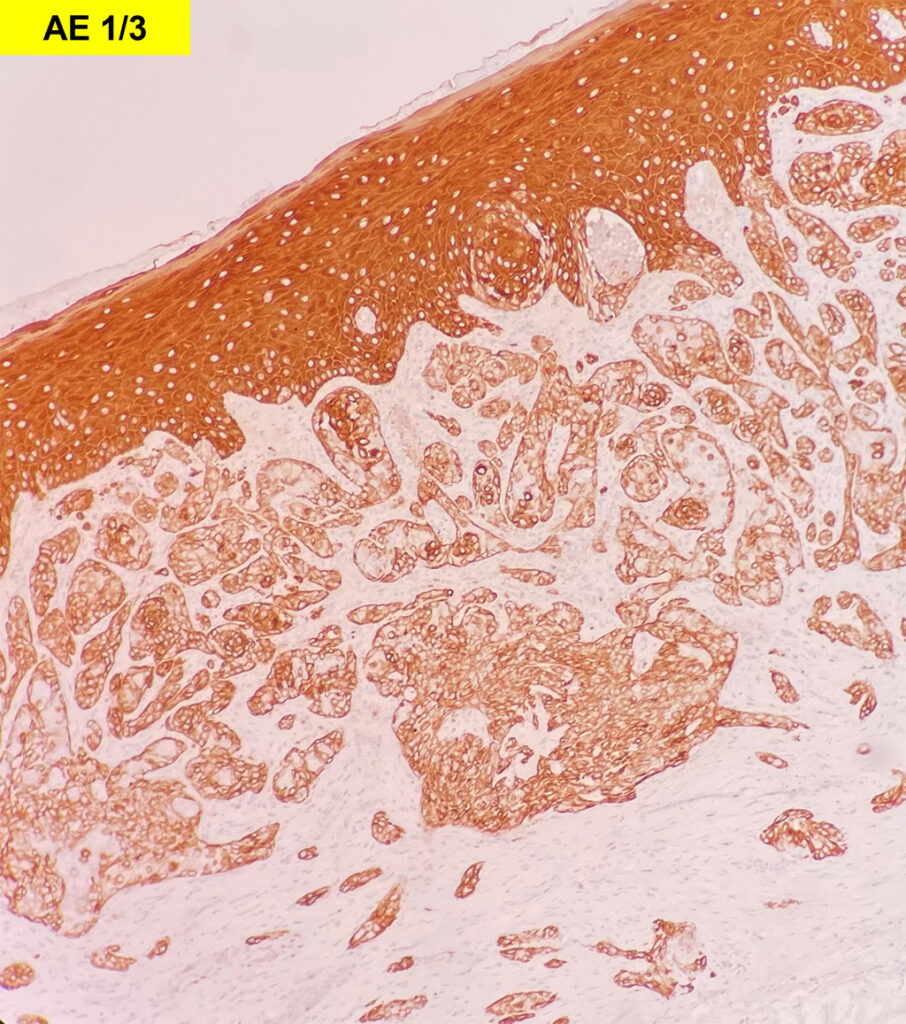
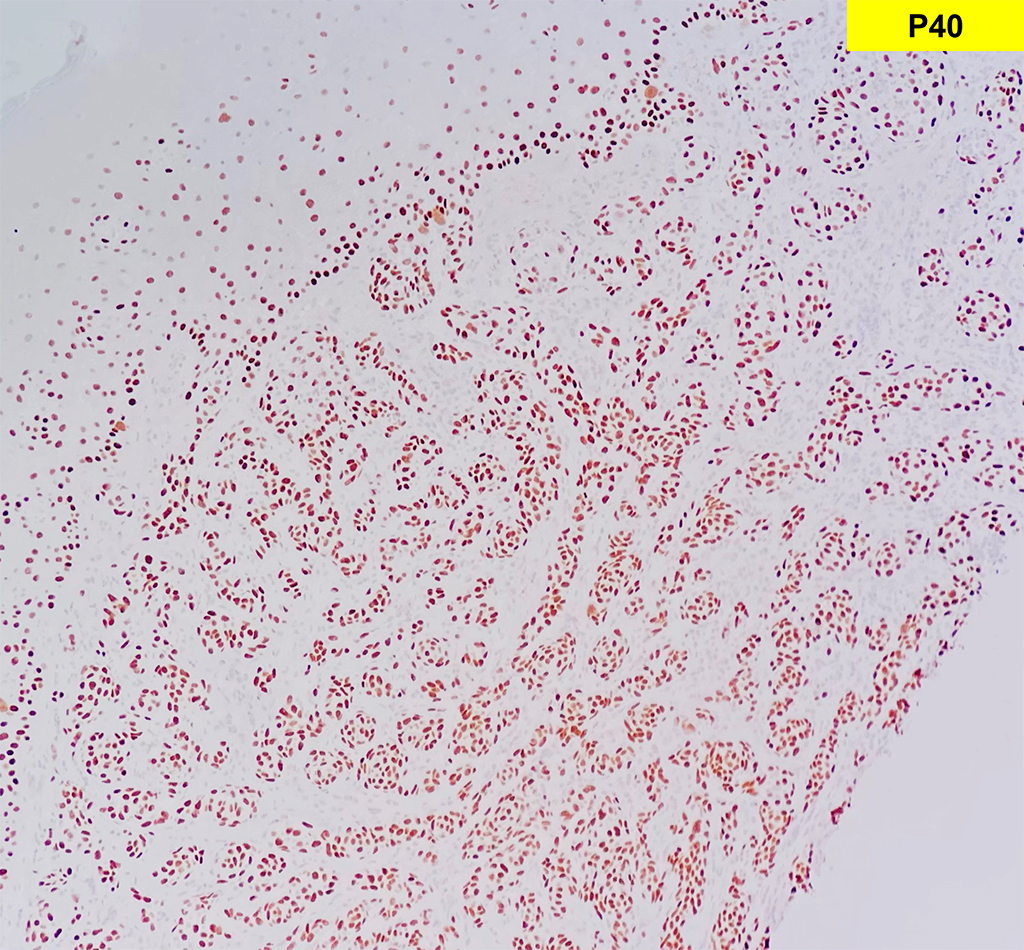
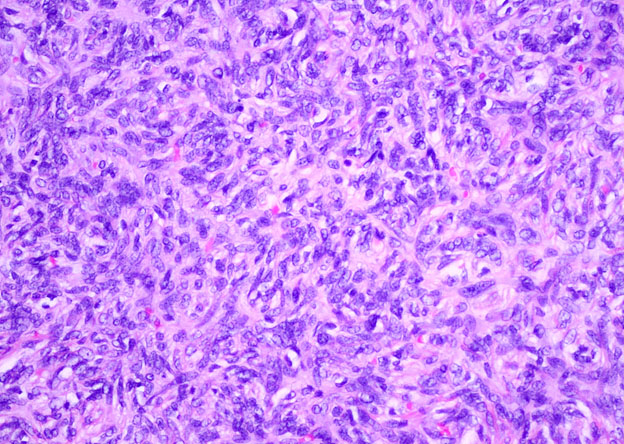
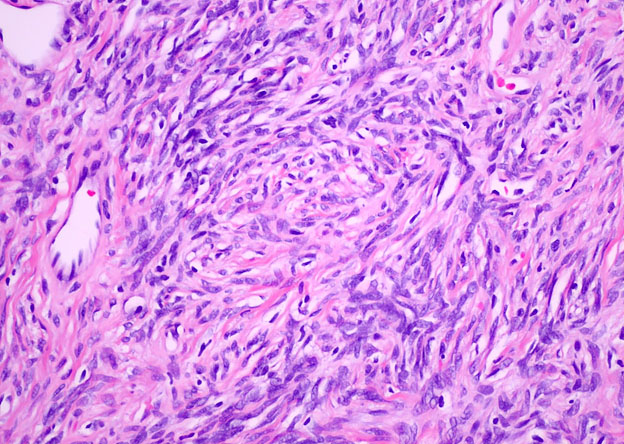
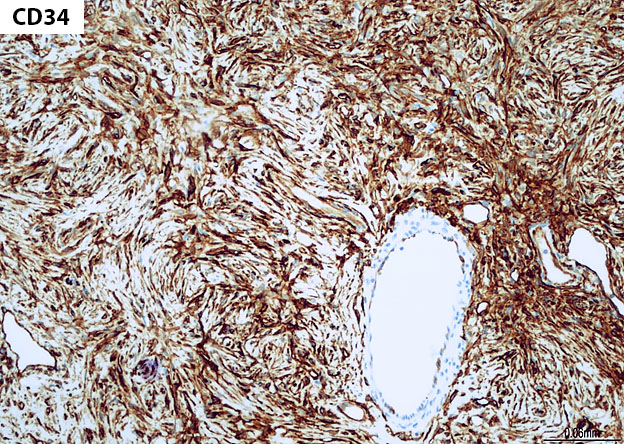
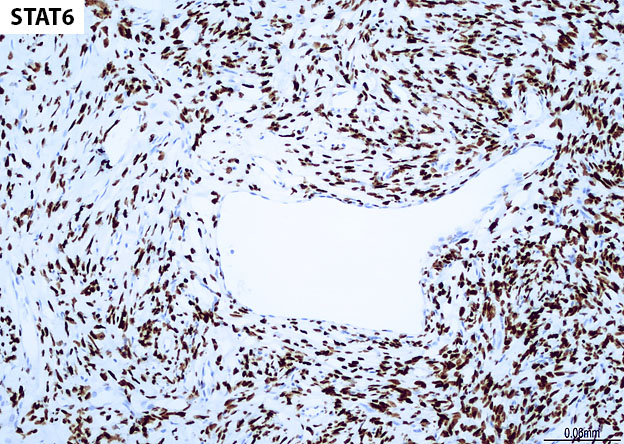
Grossly, SFTs tend to be well circumscribed and have a smooth exterior with a lobulated cut surface. Histologically, they are composed of spindle cells and show variation of growth patterns, including fascicular, storiform, or herringbone. Nuclei can be wavy and neural-like or blunt and ovoid. Frequently, there are both hypercellular areas as well as hypocellular areas with stromal sclerosis. Rope-like, linear stromal sclerosis is highly characteristic of this tumor. Spindled cells are separated by endothelial-lined, dilated, angulated, branching vascular spaces, often referred to as “hemangiopericytoma or HPC-like”, after the vessels identified in intracranial hemangiopericytomas (most of which are now known to share similar morphology and identical genetics to SFTs of other sites). The vessels range in size from capillaries to large and patulous but usually do not have muscular walls. There is no cytologic atypia within the endothelial cells. Additionally, nuclear pleomorphism is absent or limited in the spindle cells. Chromatin is usually open with inconspicuous nucleoli. Mitotic activity is usually rare. A subset of SFTs may have atypical histological features such as areas of hypercellularity, infiltrative borders, moderate to marked nuclear pleomorphism, necrosis, or >4 mitoses per 10 HPF, and are more likely to behave in a malignant fashion. While the spindle cells are positive for CD34, Bcl-2, CD99, and vimentin, nuclear expression of STAT6 is most specific – as it reflects the underlying NAB2-STAT6 gene fusion. This fusion is present in SFTs of all anatomic sites.
In most cases, complete surgical removal is curative. However, prediction of behavior based on histological criteria alone may not be accurate as SFTs may recur or metastasize even in the absence of atypical histological features. Therefore, long-term follow-up is recommended for all SFTs.
References
- Gold JS, Antonescu CR, Hajdu C, et al. Clinicopathologic correlates of solitary fibrous tumors. Cancer 2002;94:1057–68
- Fan CY, Van Hemert RL, Thomas JR, et al. Atypical solitary fibrous tumor of the larynx. Otolaryngol Head Neck Surg 2006;134:880–2
- Hasegawa T, Matsuno Y, Shimoda T, et al. Extrathoracic solitary fibrous tumors: their histological variability and potentially aggressive behavior. Hum Pathol 1999;30:1464–73.
- Rodrigues, Fernandes, et al. Solitary fibrous tumor of the floor of the mouth. J Clin Exp Dent. 2017 Sep; 9(9): e1153–e1157.
Quiz Answers
Q1 = C. NAB2-STAT6 fusion
Q2 = B. False